
CBT for Insomnia – What Techniques can be used?
January 28, 2015
rTMS – Side effects and Guidelines for use
March 19, 2015Structure of Sessions
The CBT protocol most frequently used is that developed by Morin. It provides for a treatment plan over six to ten sessions on a weekly basis. The first two sessions should focus on the clinical evaluation, which should include a 2 week use of the sleep diary. The following sessions are the actual therapy sessions. The sessions of individual therapy should last about 50 minutes, while those of group therapy should be about 90 minutes. The organisation of each session should be structured as follows:
1. Examine the sleep diary, asking the patient to give an interpretation, in order to raise awareness of the factors that may promote or hinder sleep; 2. Assess compliance to homework given; 3. Identify the difficulties encountered during practice at home and find practical strategies to promote adherence to treatment; 4. Present a new therapeutic element and then explain its rationale; 5. Illustrate, with the use of educational material, any new therapeutic element; 6. Create and review tasks to be carried out at home during the next week; and 7. Provide a written summary.
Progress should always be assessed in conjunction with the patient. Finally, it is important to convey enthusiasm and to encourage the patient during difficult phases of treatment, whilst also providing data on the success that CBT has in treating the problem of insomnia.
Individual and Group CBT
CBT for insomnia may be implemented both on an individual basis as well as in a group. There is also evidence that shows positive results of other less traditional mediums, including internet forums, telephone therapy or self-administered audio recordings.
Individual therapy can be tailored to the specific needs and circumstances of the patient, both with respect to the order as well as the form of intervention. Seeing the patient individually, it is also possible to address problems related to the disorder, which may interfere with the therapeutic process and prevent the improvement of sleep. Group therapy, on the other hand, has a better cost-benefit ratio than individual therapy, and also has a number of its own positive aspects. Patients will realise that they are not alone in their suffering, and may share their problems with other participants; the group can become a kind of social support network, and patients who are more diligent in following the instructions of the therapist may serve as a stimulus and as an example for others. Finally, the fact of being in group prevents patients from dwelling too much on personal matters, which go beyond the treatment of insomnia.
Indications of CBTi
Smith and Perlis propose an algorithm to select patients who may benefit from CBT treatment for insomnia, taking into account different aspects:
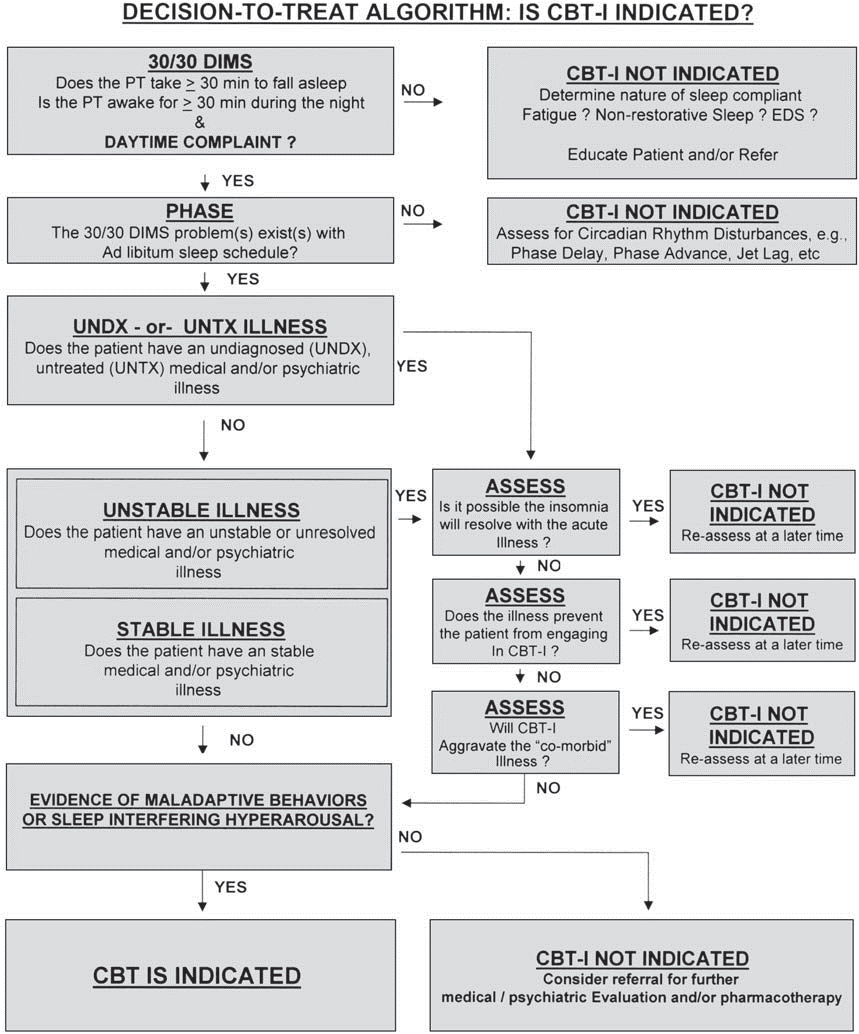
Conclusions
In conclusion, a systematic review of the literature on CBT for insomnia shows that this form of treatment leads to significant improvements in participants with chronic primary insomnia, and that the treatment package of the full range of techniques (CBTi) as outlined above, is superior to a treatment with individual components, such as relaxation training, psycho-educational programs, pharmacotherapy or placebo. In particular, CBT has shown to decrease the reliance on sleep medications without causing deterioration in sleep. Moreover it seems that the mild depression may improve due to the treatment of insomnia with CBT. CBT has also shown promise in the treatment of secondary insomnia, although not much research has been done in this field. It is hoped that the increasing popularity of CBT for the treatment insomnia will result in dramatic reductions in economic and social costs; both consequences of insomnia, as well as an improvement in the quality of life of patients suffering from this condition.

